Have you or a family member ever struggled with red, itchy skin and thought that it could be something more than just a one-time occurrence? Well, it’s definitely possible that it’s more serious than a rash or inflammation. It could be that you’re experiencing psoriasis or eczema.
Psoriasis and eczema are both quite common skin conditions, as over 8 million people in the United States are diagnosed with psoriasis, and over 30 million have some form of eczema. With such a high volume of psoriasis and eczema patients, it’s important to know the differences between the two, which can be tricky since their symptoms look similar.
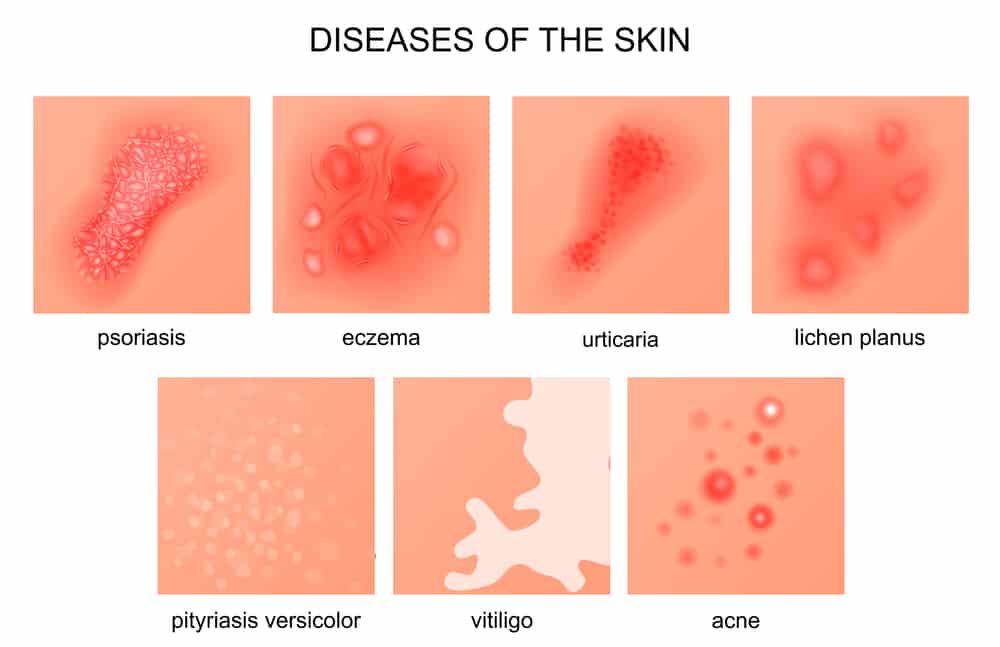
Both conditions can affect anyone at any age and can be caused by different factors. They also have different treatment options depending on the severity of the case. Keep reading to learn the signs and treatment options for both in case you suspect that you or a family member have one of the conditions. However, keep in mind that visiting your healthcare provider is the best and most accurate way to receive a proper diagnosis.
Psoriasis vs. Eczema
First off, it’s important to know what exactly psoriasis and eczema are, and how they’re classified medically.
According to GoodRx, psoriasis is classified as an autoimmune disease that causes inflammation of the skin and damage to the nails. An autoimmune disease occurs when the immune system attacks its own healthy cells. Currently, there is no established reasoning behind the development of autoimmune diseases as scientists are still researching the root cause.
There are six main variations of psoriasis, but the two most common are plaque and nail psoriasis. Those who suffer from psoriasis experience periods of inflammation to the skin that can be painful and itchy. However, they do experience phases of remission as well, so flare-ups are not always occurring.
On the other hand, eczema is a type of dermatitis according to the Cleveland Clinic. Dermatitis is a blanket-term that describes irritated skin. This irritation is usually associated with dry, itchy, rashy skin. With this eczema, damage is caused to the skin and its protective barrier, which can result in skin sensitivity and an increased chance of infections and dryness.
Since eczema can cause severe itchiness, some people itch their affected areas profusely which can lead to bleeding and even leathery textured skin. Due to itching and bleeding, eczema areas can become infected, unlike psoriasis plaques. Infections can lead to further complications down the line and create more discomfort.
While both conditions can occur at any age and develop in anyone, there are periods in life where a diagnosis is more likely. For example, eczema usually occurs earlier in life, beginning as early as six months of age. Oppositely, psoriasis developments are more likely to occur between the ages of sixteen and twenty-two.
The good news is that neither condition is contagious and both can be managed with proper care and a doctor’s diagnosis.
What Do Psoriasis And Eczema Look Like?
There are similarities in how psoriasis and eczema look on the skin, but some key differences make it easier to identify which you may have.
Psoriasis Symptoms
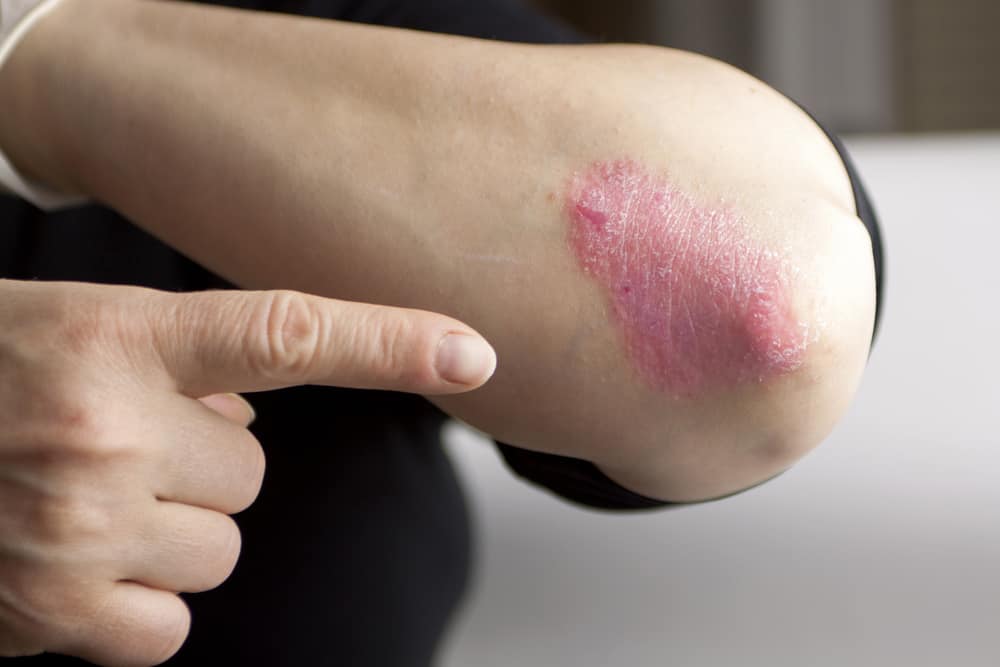
The symptoms of psoriasis vary from person to person depending on which form of psoriasis they are experiencing. Generally speaking, psoriasis presents itself as plaques of bumpy, scaly, red patches on the skin. Common areas for these plaques include the arms, legs, scalp, torso, and buttocks.
Aside from the visible plaques that form on the skin from psoriasis, some may experience changes to their nails as well. The nails may become brittle, show signs of crumbling, change in colors, and present cracking.
Eczema Symptoms
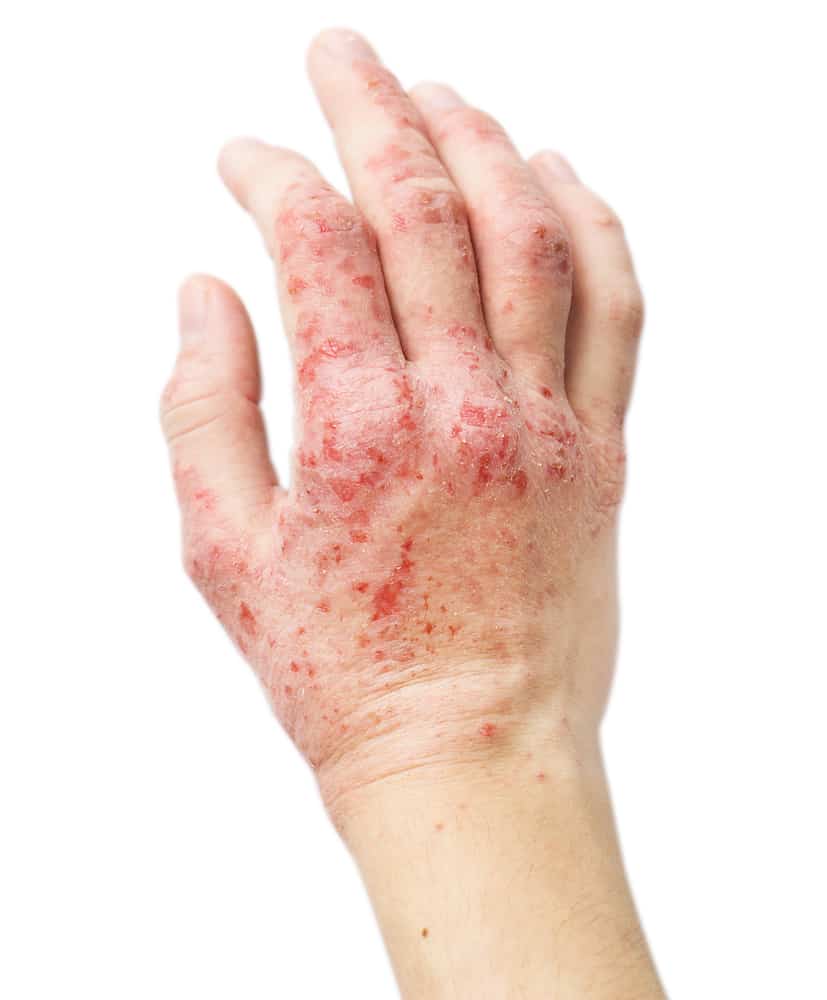
Similar to psoriasis, eczema symptoms appear as dry, itchy red patches of skin that can form anywhere on the body. There are also multiple forms of eczema, however, atopic dermatitis is the most common type and is the one that is usually referred to when people speak about eczema.
What Are The Causes And Triggers Of Psoriasis And Eczema?
As previously mentioned, both skin conditions have different sets of causes and triggers. Since psoriasis is an autoimmune disease, it’s hard to determine the exact root cause as it’s still unknown why the body begins to attack its healthy cells. Eczema also has no one known root cause, but some known triggers have been determined and can be avoided.
Triggers of Psoriasis
Triggers or contributing factors that increase the chances of developing psoriasis include:
● High-stress levels
● Cuts and scrapes on the skin
● Smoking
● Alcohol consumption
● Poor diet
● Health infections like HIV or strep throat
● Reactions to certain medications
● Genetics
Triggers of Eczema
Triggers or contributing factors that increase the chances of developing eczema include:
● Dry skin
● Stress
● Genetics
● Itchy Wool
● Fragrances
● Allergens like pollen or dust mites
To limit the chances of psoriasis or eczema, be sure to live a healthy lifestyle and avoid these triggers if you’re worried about the development and want to keep yourself and your skin smooth and healthy.
What Are The Different Treatment Options For Psoriasis And Eczema?
While psoriasis and eczema are both chronic skin conditions, they each have treatment options to manage breakouts and make periods of flare-ups more comfortable. It’s important to note that neither condition has a cure, but medications and at-home treatments can help reduce symptoms.
One option that works for both eczema and psoriasis is a topical treatment that gets applied right to the affected area(s) of the skin. These include creams, gels, and ointments.
The most common kind of topical treatment for both conditions includes some form of corticosteroids, also known as steroids. Corticosteroids aid in reducing inflammation and redness and are available in different strengths for different severities of the conditions.
There are also other treatment options for those that need stronger medications. These are typically in oral or shot forms and require a prescription from a doctor. This includes immunosuppressants for eczema which lower the body’s immune response. Acitretin is an option for psoriasis which slows down cell growth.
Alternatively, over the counter and at-home options include:
● Hydrocortisone cream to improve eczema and psoriasis
● Warm baths to lessen skin pain
● Salicylic acid helps remove extra skin cells caused by psoriasis
● Calamine for itch relief
● Coal tar for psoriasis
Again, keep in mind that it is best to seek professional medical advice for the best treatment option for yourself or a loved one.
Other Complications That Can Occur
Because of the toll these conditions take on your body, those who suffer from psoriasis or eczema are also at greater risk for developing other health complications.
Those living with psoriasis are at a greater risk for:
● Depression
● Anxiety
● Diabetes
● Inflammatory Bowel Disease
Those living with eczema are at a greater risk for:
● Asthma
● Hay fever
● Food allergies
These conditions are not guaranteed to occur but be sure to speak with your doctor if you notice any health changes that could be a result of your psoriasis or eczema.
Lifestyle Changes For Psoriasis and Eczema Flare-up Prevention
If you’re worried about the development of either disease, or if you or a family member are more prone to diagnosis, then consider making some lifestyle adjustments to lessen the chances. These changes can reduce the risk of developing eczema or psoriasis and potentially improve your flare-ups.
Healthy Diet

A diet that is high in anti-inflammatory foods can do wonders for skin health. Your skin reacts to what you put into your body, and foods high in sugar or processed ingredients can cause harm to your skin health.
To decrease your chances of developing a skin condition, consider adding more fruits and veggies to your meals or switching to a plant-based diet altogether. Fruits and vegetables are full of anti-inflammatory properties and can reduce the chances of outbreaks.
Another option for diet is the Autoimmune Protocol Diet (AIP). This diet focuses on eliminating foods that can make symptoms of autoimmune diseases worse. The AIP diet incorporates foods and ingredients that are good for gut health and reduce inflammation and has been proven to increase ‘good days’ for those who suffer from autoimmune diseases.
Practice Good Skin Care
A proper and consistent skincare routine can help prevent both psoriasis and eczema outbreaks. The number one priority when it comes to skincare for these conditions is keeping your skin moisturized. As a general rule, it’s best to use a thick cream, rather than a thin lotion, so your skin can soak up as much hydration as possible.
If you don’t currently have a skincare regime, speak with your doctor or a dermatologist to determine the best products for your skin type. It’s important to find products for your skin that don’t cause irritation or damage. A good rule of thumb is that if a product burns, you should stop using it immediately. A proper skincare routine will help keep your skin in good condition and prevent the chances of inflammation from occurring.
Stress Management

Seeing as stress is a potential trigger for both psoriasis and eczema, it’s important to keep your stress levels under control to limit your chances of development. It can be hard to cope with stress, especially during traumatic life situations. However, with the right tools, stress management is possible and crucial when it comes to preventing skin conditions.
Consistent Sleep Schedule
When managing any kind of condition, it’s important to get the right amount of sleep to give your body and immune system the energy it needs to function properly. When your body is overtired, it causes inflammation that can worsen psoriasis and eczema symptoms.
Unfortunately, the uncomfortable symptoms from both eczema and psoriasis can make it difficult for you to relax and achieve a good night’s rest. Luckily there are a few steps you can take to prevent yourself from being itchy and uncomfortable all night long.
Start by establishing a sleep schedule and sticking to it. Find an activity or two that helps you wind down and puts you in a relaxed state, like reading or meditating. Be sure to moisturize before you lay down for the night to help manage some of the itching and pain from your condition, and wear pajamas made of cotton or another material that won’t irritate your skin.
You should also work to make your bedroom an environment that promotes a good night’s rest. That means making sure that the temperature is not too hot or too cold, as either can make you prone to itchiness. The more that you can calm your mind, the easier it will be for you to fall and stay asleep.
Limit Drug And Alcohol Use
As previously noted, alcohol and smoking can be triggering for psoriasis and eczema and worsen flare-ups. These substances can dehydrate your skin, trigger inflammation throughout the body, and hinder the effectiveness of your medications.
If you’d like to limit your chances of a skin condition diagnosis, consider limiting your alcohol and drug use to keep your body performing well. Talk with your doctor if you’re having trouble quitting these substances, and always be honest with them on how much you indulge in drugs or alcohol and how they make you feel. This will help them understand how to best manage your psoriasis or eczema.
The Role Of Family Health History In Psoriasis and Eczema
Have you ever gone to the doctor and had to fill out one of those family health history forms? Well, there’s an important reason for that. Informing your doctor of your family health history can help determine your chances of developing certain hereditary conditions.
A family history of either psoriasis or eczema greatly increases your chances of developing them. Doctors and scientists are unsure of the reasoning, but they have done studies that show those with a family health history of either condition are more prone to developing it than those without a family history of the disease.
If you know that either of these conditions runs in your bloodline, then let your own doctor and your kids’ doctors know so that they can run any necessary tests and ask specific questions in the case of a potential diagnosis.
Summary of Psoriasis vs. Eczema
Overall, psoriasis and eczema are very similar in the sense that they are both skin conditions that cause discomfort. However, the main difference is that psoriasis is an autoimmune disease while eczema is not. Neither conditions have a cure, but with proper care and attention, symptoms and breakouts can be limited and easily managed.
Above all, speak with your doctor if you suspect that you have a skin condition so that they can properly diagnose you and help you determine a treatment plan that will work for you and your needs.

